Rosacea is such a common presentation that I see in my private Dermatology practice. Despite how common it is, Rosacea is a tricky beast! It is a condition that needs good understanding of its underlying pathogenesis (ie. what is causing it), and acceptance of the fact that there is unfortunately no cure. It’s all about finding a combination of skin care products and medical treatments that you can use as ongoing maintenance, to get your skin back on track and keep it looking its best.
Rosacea; let’s start with the basics!
You can read plenty of information about Rosacea on the internet (Dermnet NZ is a reliable source to read), however I think the key thing to know and understand, is that there are a number of different aspects and subtypes of Rosacea, and the most common ones are:
Papulopustular Rosacea
In short, this is the ‘acne like’ spots occurring classically on the cheeks, in Rosacea. Largely speaking, disturbances in the skin microbiome (natural skin flora) play a key role in this, with an overlay of secondary inflammation. So management overall involves tackling the ‘bugs’ and the inflammation.
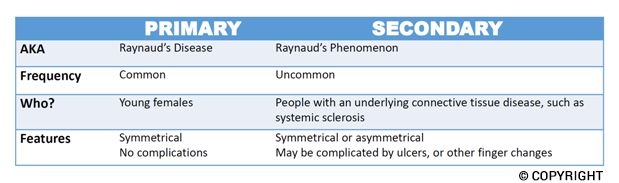
Erythro-telangiectactic Rosacea (ETR)
This involves background redness (which is due to small dilated and permanently visible superficial blood vessels in the skin) and/or episodes of flushing. ETR often makes the skin very easily irritated with burning / stinging. Triggers such as alcohol and heat are common, and sun protection is also a key aspect to management.
Ocular Rosacea
Eye symptoms such as a burning / stinging, occur in a proportion of those with Rosacea. This can sometimes be mistaken for hayfever or other causes of eye irritation.
If you know this, you’re well on your way to understanding all you need to about Rosacea. Why? Because each of these aspects has slightly different underlying pathogenesis (ie. what is causing it) and so needs to be considered a little bit separately when it comes to treatments.
Now onto treatment…
First, avoid things that trigger your skin
Most people with Rosacea will have consciously or subconsciously worked out what makes their skin ‘flare’. Other times it can be a bit of trial and error. Ultimately though, in the end you will know your skin much better than anyone else, as you are the one living its ups and downs on a daily basis.
Avoiding these triggers is a vital part of managing and improving your skin in Rosacea.
Common triggers for Rosacea include:
Papulopustular component (‘pimples’)
- Comedogenic products; comedogenic products are often thick products that ‘block pores’, such as thick moisturizers, comedogenic makeups and sunscreens.
Erythro-telangiectatic component (easy irritation and facial redness)
- Irritating products; acidic, astringents, toners, SLS (sodium lauryl sulfate) in facial washes
- Food / beverage; alcohol, spicy foods, hot foods, citrus, and some less common such as cheese, histamine containing foods
- Sun and heat
Skin care products in Rosacea
Avoiding irritation / redness
Skin care for your face when you have Rosacea can often be tricky, as your skin will likely be quite sensitive and easily irritated. Overall, providing specific advice about which products to use is impossible, as everyone’s ‘sensitivities’ will be a little different, and it’s usually a matter of trial and error to find what works for your skin. La Roche Posay, Cerave, Cetaphil and Avene tend to have some useful products for sensitive skin, but there are lots of good options out there. Avoiding fragrances is important, as is sticking to a cream based non-foaming facial cleanser and/or micellar water for sensitive skin.
Avoiding the ‘spots’ / pimples
As well as being prone to irritation, you may also be prone to ‘break outs’ (papulopustular rosacea) which means choosing non-comedogenic products which don’t promote acne-like ‘break outs’ is also important to consider. For makeup, using a mineral foundation can be useful, and these days there are lots of great liquid mineral foundations readily available.
And to make things even more challenging, the sun is a common trigger for many aspects of Rosacea, so wearing sunscreen is often very important; and yet choosing a sunscreen which doesn’t irritate your skin and/or contribute to acne-like ‘break outs’ is tricky!
Advice
So, there are many things to consider and try.
I have tried and tested a lot of products over many years. I frequently meet with various representatives from cosmetic and cosmeceutical companies to keep me up to date. And importantly I’ve learnt an enormous amount from my many patients with Rosacea. I routinely share this with my patients during Rosacea consultations, as making sure you land on a good, non-irritating and non-comedogenic skin care routine is vital to beating your Rosacea.
Medical treatments for Rosacea
Ultimately, I think it’s vital to understand that no matter what changes you make to your general skin care routine, many people with Rosacea will need a good medical treatment plan alongside that, to improve their skin. Accepting and understanding this is important – don’t sweat it, it’s really normal.
As I mentioned above, each of the subtypes of Rosacea is tackled slightly differently in terms of medical treatments, and if you see me about your Rosacea, we will go through that in detail.
Managing Rosacea from the “inside out”
One aspect that can sometimes be overlooked in Rosacea management, is the link between the skin and gut microbiome and the role it plays in Rosacea. For example, sometimes heart burn / reflux, can be linked to Rosacea. Probiotics and ingredients such as Nicotinamide may help.
So, tackling things from the ‘inside out’ can be very useful in some people.
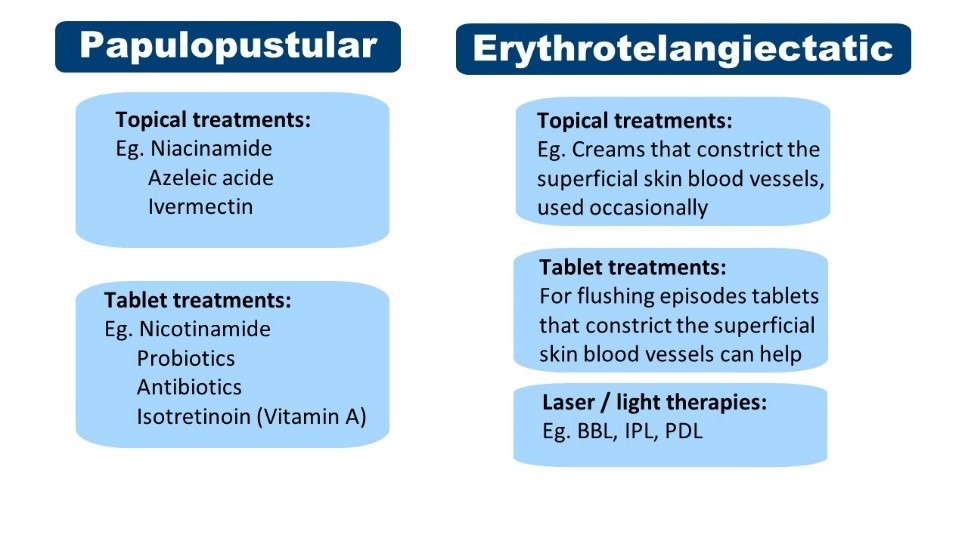
Prescription treatments
This table summarises some of the options we use as Dermatologists. The combination and order of treatments used for your Rosacea will need to be personalised and tailored to your individual Rosacea presentation.
Will my Rosacea come back?
Rosacea tends to be a chronic condition that waxes and wanes over many years. You will have periods of time where your skin is easy to manage, and then others where it all flares up and you feel like you’ve gone back to square one. Understanding this from the outset, and doing your best not to let those ups and downs affect your mental health too much is vital.
My goal in Rosacea is always to
- Explain everything I can about the condition to help you
- Give the best advice I can about general skin care products
- Prescribe an initial ‘active treatment’ plan to clear your skin up
- Move to a ‘maintenance’ phase of treatment; to keep your skin clear most of the time, with a backup plan up our sleeve, for those times when things flare up again!
Managing Rosacea is challenging, and can take time and persistence. However this only makes the reward even greater when we successfully clear your skin.
Written by AProf Amanda Saracino
© 2023 AProf Amanda Saracino